Sleep Disorders
Learn everything there is about sleep disorder types, causes, risks, symptoms, tests, treatments and support. We are here to help you sleep better!
Learn everything there is about sleep disorder types, causes, risks, symptoms, tests, treatments and support. We are here to help you sleep better!
Many people sometimes struggle to get enough rest. A variety of elements, such as stress or a hectic work agenda, can interfere with sleep. Now and then, factors like sickness, travel, or a temporary change to one’s usual schedule might lead to sleep difficulties. When sleep problems begin to consistently interfere with your daily life, it could indicate the presence of a sleep disorder.
Sleep disorders should be taken very seriously because they can cause much more than daytime sleepiness. If not addressed in a timely and proper manner, they will take a toll on your mental and physical health. Poor sleep can lead to memory problems, weight gain, irritability, and much more. Lack of sleep will also severely impact your energy and mood.[1]
If you have a sleep problem, there is no need to simply accept your fate and live with it. Learn what you can do to get a better night’s sleep and improve your overall health and wellbeing.
Having a sleep disorder means you are suffering from a condition that regularly impacts your ability to get enough shuteye. It is normal to occasionally have a hard time to fall asleep. However, it is not normal if you have regular sleep problems and you wake up every day sleepy and exhausted.
Being sleep deprived can severely affect every aspect of your life. When you sleep badly at night, you will wake up dead tired in the morning, and the little energy that you have left will be quickly drained by your daily activities and obligations. Then, even though you are exhausted, you still can’t fall asleep at night. Before you even notice, you are trapped in a vicious cycle that slowly consumes you and takes a toll on your mood, energy, efficiency, and ability to handle stress.

Sleep problems mustn’t be ignored because they can lead to severe physical and mental health damage. Lack of sleep will lead to weight gain, impaired job performance, memory issues, and so on.[2] Due to sleep deprivation, you won’t be able to focus and stay alert which increases your risk to cause an accident.[3] Your social life may also suffer by putting a strain on your relationships. In order to stay healthy, you need quality sleep. Always keep in mind that quality sleep is not a luxury but a necessity.
Even though you have struggled with sleep problems for a very long time, it is never late to do something about it. In order to sleep better, it is important to track your symptoms and sleep patterns. Implementing healthy changes to your daytime habits, bedtime routine[4] and sleep-wake schedule should also help. If self-help doesn’t work, it is time to turn to medical practitioners who specialize in sleep medicine. A sleep specialist will be able to help you identify the cause of your sleeping problem, as well as way to improve your sleep and quality of life.
Since everyone experience a sleeping problem occasionally, it may be hard to determine if your sleep troubles are just a minor annoyance or a sign of a more serious condition. In some cases, sleeping difficulties can also be a sign of an underlying medical condition.
If you experience the following symptoms, you should look into your sleep problem more closely.
If you experience any of the above symptoms every day, we have bad news – you may be dealing with a sleep disorder. The more you answered affirmatively, the more likely it is that you have a serious problem.
There are over 96 different diagnosable sleep disorders. However, the most common are insomnia, sleep apnea, restless leg syndrome, and narcolepsy.
A disrupted circadian rhythm causes most sleep disorders.[5] Circadian rhythm is our body’s internal clock that is responsible for regulating our 24-hour sleep and wake cycle. Natural light significantly influences our circadian rhythm. When there is less light, a hormone that makes us sleepy, melatonin, releases. In the morning, the release of melatonin is decreased which signalizes our brain that it is time to wake up.[6]
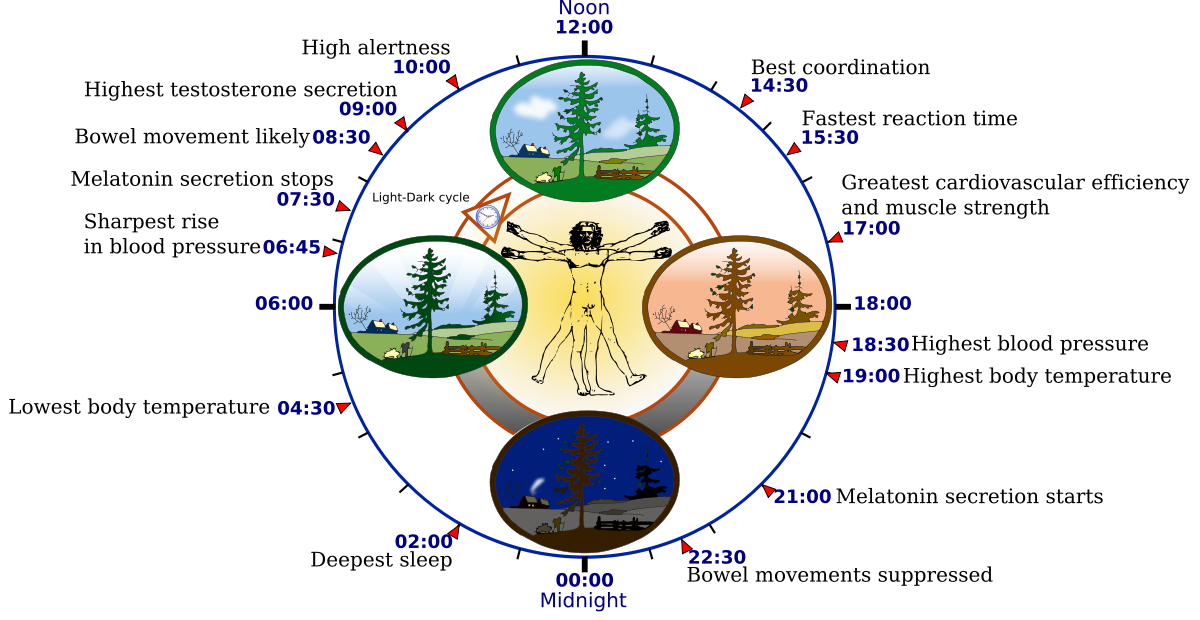
Source: Wikipedia
If your circadian rhythm is disrupted, you will feel sleepy at inconvenient times, disoriented and irritable. Circadian rhythm disruption can be caused due to many reasons and even other diseases such as depression, bipolar disorder, and seasonal affective disorder also known as winter blues.
The ICSD has classifies sleep disorders into six major categories – insomnia, sleep-related breathing disorders, central disorders of hypersomnolence, circadian rhythm sleep-wake disorders, parasomnias, and sleep-related movement disorders.
Insomnia is the inability to fall or stay asleep at night. This sleep problem can be caused by stress, jet leg or another health condition. Medications that you take also affect your sleep. Consuming too much coffee and other caffeinated beverages will also cause insomnia. Mood disorders such as depression and anxiety can also cause insomnia.
People who suffer from insomnia have the following symptoms:
Insomnia can be primary and secondary. Primary insomnia is not directly associated another health condition or disease. Secondary insomnia means that your sleep problems are caused by another medical condition such as asthma, depression, arthritis, heartburn, pain and so on.
Insomnia can also be acute and chronic. Acute insomnia is short-term and usually lasts from one night to two weeks, while chronic insomnia is long-term and can least from three nights to a month or longer.
Acute insomnia can be caused by many reasons, commonly due to severe life stress. It can also be caused by physical or emotional discomfort, as well as an illness. Environmental factors such as noise, bright light, or extreme temperatures can also disrupt your sleep. Chronic insomnia, among other, can be caused by depression, chronic stress, and pain.[7]
In order to diagnose insomnia, it is essential to talk to your doctor. Diagnosing this condition requires a physical exam, and checking your medical and sleep history. Keeping a sleep diary and tracking your sleep patterns, as well as how you feel during the day is often required to diagnose insomnia. If you are sleeping with your partner, your doctor may have to interview him or her to find out more about your sleep quality. It is not rare that you will have to visit a sleep center and undergo special tests.
In most cases, acute insomnia doesn’t require treatment. Individuals suffering from mild insomnia can often alleviate the symptoms by practicing good sleep habits.[8] If sleep habits don’t work, your doctor may prescribe you some sleeping pills. Using over-the-counter sleeping pills is not wise because they have many unpleasant side-effects the following day. Keep in mind that taking sleep drugs is not a long-term solution to your problem. As you build tolerance, all sleep meds lose their effectiveness over time.[9]

To treat chronic insomnia, your doctor must determine the underlying cause that is causing it. If insomnia is persistent, your physician may recommend behavioral therapy. Behavioral therapy focuses on helping you to change behaviors that can worsen insomnia as well as learning new behaviors that promote better sleep.[10]
Sleep apnea is a very common and treatable sleep disorder. Individuals suffering from this condition wake up frequently during night because their breathing temporarily stops. People with sleep apnea often don’t remember waking up, but they will certainly feel dead tired in the morning and notice a decrease in their productivity. Sleep apnea is a health condition that must be taken seriously, especially because it’s potentially life-threatening. Sleep apnea can be obstructive and central.
Obstructive sleep apnea happens because something is partly or completely blocking your upper airway during sleep. This causes your diaphragm and chest muscles to work harder to open the obstructed airway and pull in air. In these cases, breathing resumes with a snort, loud gasp or sometimes a body jerk.[11] Although you don’t sleep well, you probably won’t be aware of any of this. If obstructive sleep apnea is not treated, it will continue reducing the flow of oxygen to vital organs which may lead to irregular heart rhythms.
Signs of obstructive sleep apnea include the following:
Symptoms in children are different than in adults. They include the following:
Individuals who share their bed with someone are lucky because their partner will probably notice these symptoms. Parents who suspect their children may have sleep apnea should check them overnight.
Right now, the most reliable sleep apnea self-tests are the Epworth Sleepiness Scale[12], the Berlin Sleep Questionnaire[13], and the STOP-BANG test.
The STOP-BANG survey[14] is a self-test that can assess the chances of having sleep apnea. However, to get a proper diagnosis, you must see a doctor. Your doctor will decide if you need further evaluation. If you have obstructive sleep apnea, additional testing will be necessary.

Look out for the following five criteria that increase your risk of sleep apnea:
High BMI: Being overweight or obese doesn’t necessarily mean you will get sleep apnea. However, extra weight significantly increases your risk because it puts added pressure on your respiratory system, and makes it harder to breathe at night.
A Large Neck Circumference: If a man has a neck that is 17 inches or greater in circumference, his risk of sleep apnea is increased. A woman whose neck measures 16 inches or greater are also at risk. Risks are increased due to weight of the neck that pushes on the airway during sleep.
Snoring: Loud snoring should be worrying because it is a first indicator that you are not breathing freely.
Smoking and Alcohol: Since alcohol relaxes throat muscles, they may obstruct your airways easier. Smokers are also at risk because the tobacco irritates and inflames the upper airway.
A Small Airway: If your upper airways are naturally smaller, you may have troubles breathing at night.
As you can notice, you are more likely to get sleep apnea if you are overweight and have a thick and large neck. Also, this condition is more common among men that are more than 50 years old.

It is obvious that you cannot change the size of your neck and airways. However, you can make certain lifestyle changes, such as losing some weight and reducing cigarettes and alcohol to decrease your risk for sleep apnea.
Apart from smaller airways in their throat, nose, and mouth, people with enlarged tonsils, uvula and soft palate are also at hogher risk of OSA.[15] A tongue that is larger than average can sometimes also block the airway. Lastly, a deviated septum can cause obstructive sleep apnea. Apart from the mentioned, other risk factors include smoking, diabetes, hypertension and heart disease.[16]
Diagnosing this sleep disorder requires a physical exam, and checking your medical and sleep history. Your bed partner will most likely be asked for more information about your sleep habits. In many cases, a sleep study will have to be done at your home or in a sleep center. A sleep study requires wearing devices that will monitor your air flow, breathing patterns, heart rate, muscle activity, brain activity and similar. The study is necessary in order to determine how many times your breathing was impaired during sleep.[17]
In 90% of the cases, losing some weight will make a difference. People who suffer from sleep apnea should avoid alcohol and sleeping drugs because these tend to cause your airway to collapse during sleep. It is not recommended to sleep on your side. If you have problems with nasal congestion, using nasal sprays is recommended to facilitate breathing.
Standard treatments include positive airway pressure therapy, oral pressure therapy, oral appliances, surgery and behavioral therapy.
CPAP machine is a device that consists of a mask and an air blower. Since the air blower continuously forces air through the nose or mouth, it will prevent your upper airway tissues from falling down during sleep. A similar device to CPAP is BPAP that has two levels of air flow.[18]
People who suffer from mild sleep apnea can use oral devices such as dental or mandibular appliances that will prevent their tongue from blocking the throat. These devices help the airway stay open during sleep.
Surgery is recommended to people who have a deviated septum, a small lower jaw, adenoids that need to be removed, enlarged tonsils, or extra or misshapen tissue that blocks proper airflow through the nose and mouth.
An oral appliance looks similar to a sports mouth guard or orthodontic retainer. This oral appliance can help you reduce snoring and ensure your airways are open during the entire night.
Obstructive sleep apnea is typically treated with continuous airway pressure therapy or CPAP. This type of therapy requires wearing a mask that blows air into the airways to keep them open. The mask is worn only during sleep. However, most people find wearing this mask uncomfortable. If you can’t tolerate CPAP, maybe an oral appliance is more suitable for you.
Oral devices can be prescribed to patients who suffer from mild sleep apnea. These oral devices are custom-made by dentists. Your dentist will show you how to wear and properly clean it. Although oral appliances are not effective as continuous airway pressure therapy, many people prefer using a dental device because it’s much more comfortable and has minimal side effects.
Obstructive sleep apnea affects more than 18 millions of American adults. Since this sleep disorder continuously grows and affect more and more people every day, sleep scientists are doing their best to come up with new treatments that will help patients sleep better and live a better and more productive life. The latest treatments for OSA are hypoglossus nerve stimulation and expiratory positive airway pressure therapy.
This type of treatment for sleep apnea was approved by the FDA in 2014. It includes implanting a small device in the chest that can be turned on and off by the patient. During sleep, the device monitors the patient’s breathing and stimulate the hypoglossus nerve to keep the upper airway open. Since this type of therapy is invasive, it is recommended only when patients are not helped by standard OSA treatments.
The EPAP therapy consists of placing disposable adhesive valves over the nose when you sleep. The device ensures the patient’s airways are open during inhaling and exhaling.
Central sleep apnea is rarer than obstructive sleep apnea. Individuals with this disorder suffer from disrupted breathing during sleep. Unlike obstructive sleep apnea, in central sleep apnea, the breathing stops because of the way the brain functions. The brain fails to tell your muscles to breathe for a short amount of time. This type of sleep apnea is often associated with severe health problems and diseases in which the lower brainstem is affected.
Conditions that may be associated with central sleep apnea are congestive heart failure, hypothyroid disease, and kidney failure. Some neurological diseases such as Parkinson’s and Alzheimer’s disease can also cause central sleep apnea. Damage to the lower brainstem caused by an injury or a stroke may also lead to central sleep apnea. Symptoms, diagnosis, and treatment are the same as for obstructive sleep apnea.
The most familiar central disorder of hypersomnolence is narcolepsy. These sleep disorders are also known as excessive sleepiness disorders because they are characterized by daytime sleepiness that is not caused by disturbed night sleep or misaligned inner body clock.
Poor sleep habits typically cause excessive sleepiness. In order to handle this problem efficiently, it is recommended to review your routines, schedules, and the environment you’re sleeping in. This way, you may identify a potential problem and make some adjustments to improve your sleep.
The primary cause of excessive sleepiness is insufficient sleep. Sleeping less than the recommended 8 hours per night will lead to irritability, drowsiness, and stress. Sleep deprivation will also cause you to feel moody and underproductive, especially as your slept debt accumulates over time.
If you practice healthy sleep habits such as avoiding caffeine and blue light in the evening and sticking to a regular bedtime schedule, the problem may be in your sleep quality. Poor sleep quality means your sleep is interrupted or not deep enough to have a restorative effect.
If you have a problem with frequent waking up during the night, you should practice relaxation, avoid electronic devices before bed and make sure your bedroom is dark, comfortable and reasonably cool.
If you believe your sleep is interrupted during the night but you still wake up tired in the morning, you may have sleep apnea, which significantly reduces sleep quality.

Excessive sleepiness can also be caused by a change in schedule that is caused by tight work schedules or school responsibilities. Shift workers are the ones that are at highest risk for excessive sleepiness. Since their sleep time is not in hours when it should be, they experience difficulties falling asleep. Our body needs time to adjust to a new sleeping schedule. Unfortunately, sometimes, when their body adjusts, their work schedules change again, and they are back at the beginning. That is why shift workers have so many problems with sleep.
If you’ve tried to improve your sleep habits and still experience excessive daytime sleepiness, you should talk to your doctor or ask for a referral to a sleep specialist.
Certain medications can be used to address daytime sleepiness. Drugs for excessive sleepiness are meant to increase your level of wakefulness and alertness. However, it’s still vital to hold off on driving and doing anything that could be potentially dangerous until you see how the meds work for you.
Narcolepsy is a sleep disorder that is characterized by uncontrollable daytime sleepiness. This sleepiness is caused by a dysfunction of the brain mechanism that controls sleeping and waking. An individual suffering from narcolepsy feels like he is experiencing sleep attacks in the middle of working, talking and driving. The sleep attacks can occur during any time of the day and during any activity.
Normal sleep cycle consists of five stages of sleep. During those stages, a person traverses from light sleep to deep sleep and REM stage. Rapid eye movements or REM sleep typically occurs 90 minutes of deeper sleep stages.[23] However, if you suffer from narcolepsy, your REM sleep will occur almost immediately after you fall asleep, as well periodically during the waking hours. In REM sleep we experience dreams and muscle paralysis, which may explain some of the symptoms of narcolepsy.
This sleep disorder usually begins when a person is between 15 and 25 years old. However, it can become apparent at any age. Narcolepsy often goes undiagnosed and due to that untreated.
The causes of narcolepsy are unknown. Sleep experts have discovered that narcolepsy with cataplexy is caused by the loss of a chemical in the brain called hypocretin. Hypocretin is a chemical compound that is responsible for keeping us awake and alert. It also helps to regulate our inner body clock. Without hypocretin, it is hard or almost impossible to stay awake. The person suffering from narcolepsy also experiences disruptions in the normal sleep-wake cycles. Most likely, narcolepsy is caused by multiple factors that disrupt normal neurological functioning and REM sleep disruption.[24]
Symptoms of narcolepsy include uncontrollable daytime sleepiness, cataplexy, hallucinations and sleep paralysis.
Excessive daytime sleepiness occurs on a daily basis, no matter if a person with narcolepsy had sufficient sleep the previous night. People suffering from narcolepsy also report a lack of energy and concentration, memory lapses, a depressed mood and extreme exhaustion.

Cataplexy is a sudden loss of muscle tone that manifests as a feeling of weakness and loss of muscle control. Depending on the muscles involved, it can cause a number of issues, from slurred speech to total body collapse. This symptom is often triggered by intense emotions such as laughter or anger.
Hallucinations are mostly visual, but sometimes other senses may be involved. Lastly, sleep paralysis affects temporary inability to move or speak while falling asleep or waking up. It occurs in episodes and lasts a few seconds or several minutes.[25]
In order to diagnose narcolepsy properly, the patient must undergo a physical exam. Medical and sleep history also must be checked. Two specialized tests for narcolepsy are polysomnogram test and multiple sleep latency test. The polysomnogram will help establish abnormalities in the sleep cycle and find out when if REM sleep occurs at abnormal times. The multiple sleep latency test is performed during the day, and it is used to measure an individual’s tendency to fall asleep.
Currently, there is no cure for narcolepsy, but there are medications and behavioral treatments that can relieve the symptoms so affected individuals can lead a normal and productive life. Sleepiness is treated with stimulants based on amphetamine. Abnormal REM sleep symptoms are treated with antidepressant drugs. Pharmacologists have recently developed a drug called Xyrem that helps people who suffer from narcolepsy with cataplexy have a better night’s sleep and feel less sleepy during the day.[26]
Every person has unique sleeping needs. While some need eight to nine hours of sleep to feel refreshed in the morning, other feel great with just six hours of sleep per night. If you sleep more than ten hours every night and have a couple of long naps during the day, and you still feel sleepy and tired, you are probably suffering from idiopathic hypersomnia, otherwise known as extreme sleepiness.
People with idiopathic hypersomnia suffer constant or frequent episodes of extreme sleepiness. Extreme sleepiness is usually caused by another sleep disorder or medical condition such as narcolepsy, obstructive sleep apnea, REM sleep disorder, and so on.
If getting extra sleep doesn’t alleviate your sleepiness, you should consult with a doctor or a sleep specialist about the duration and intensity of your symptoms. You most likely suffer from idiopathic hypersomnia if your symptoms last at least six months, your polysomnography results are normal and if your condition is not caused by another medical or mental disease or a head injury.
The most common treatments for this sleep disorder are stimulant medications. However, these medications are not a substitute for sleep. People with idiopathic hypersomnia often sleep longer than other people, even when they are using such drugs.
Circadian rhythm sleep disorders affect the timing of sleep. People with these disorders are unable to go to sleep and awaken at times commonly required for work and school or other social needs. Among the most common circadian rhythm sleep disorders are non-24h sleep-wake disorder, shift work disorder, delayed sleep phase disorder.
This sleep disorder affects the normal 24-hour regulation and synchronization of our circadian rhythm or inner body clock. Since light mostly regulates sleep and wake cycle, non-24 sleep-wake disorder is a common sleep issue in blind people. Due to the lack of light information received from the eyes, their internal body clock cannot regulate the 24-hour day-night cycle properly.
As a result, their internal body clock returns to a non-24 hour period, characterized by fluctuating periods of good sleep, poor sleep and excessive daytime sleepiness. Although this sleep disorder mostly affects blind people, it can also occur in healthy people, but it is typically temporary and caused by stress, hectic schedules and similar.
Shift work sleep disorder occurs when your work schedule and your inner clock are out of sync. People suffering from this disorder have to work night shifts or rotating shifts. The primary problem is that you are forced to be awake when you should sleep and vice versa. A problem develops when you have trouble sleeping or you have trouble staying alert when you are supposed to be awake.

If you are sleep deprived, you may have a hard time struggling with sleepiness on the job. This may also affect your productivity and increase the risk of injury.[27]
The best way to reduce the impact of shift work on your shuteye is to take regular breaks. If possible, try to minimize the frequency of shift changes. When you have to change shifts, request one that is later rather than earlier because our body adjusts easier if we go forward in time. Try to regulate your circadian rhythm by increasing light exposure at work and limiting it when it’s time to sleep.
If you have control over your work schedule, you can do some things to make the adjustment easier. For example, if you often work night shifts, try to keep the same sleep and wake schedule each day, even when you have a day off. This will help you improve your sleep quality and regulate your circadian rhythm. Proper sleep is vital for staying alert at work during your shift.
If you often rotate shifts, rotate them clockwise for easier adjustment. For example, go from a day shift to an evening shift and then to a night shift. Rotating shift the other way or without a pattern will disrupt your sleep. It is also important to adjust your sleep and wake time gradually.
Delayed sleep phase disorder is a health condition characterized by a delayed inner clock. As a result, people suffering from this disorder go to sleep and wake up much later than other people. It is important to have in mind that this is not a preference. It is a disorder that disables you to keep normal hours. People with delayed sleep phase disorder can’t make it to their morning classes and can’t keep a 9-to-5 job. No matter how hard they try, these individuals can’t fall asleep earlier than 2 a.m. to 6 a.m.
A very interesting fact is that when they are allowed to keep their own hours (such as during a vacation or a school break), their circadian rhythm is restored. This sleep disorder is mostly experienced by teenagers, and most of them overgrow it with age.[28]
If a person continues to struggle with a delayed inner clock, light therapy and chronotherapy are recommended and mostly helps.[29]
Jet lag is a temporary sleep disruption that occurs when you travel across time zones. Symptoms include daytime sleepiness, fatigue, headaches, stomach problems, and insomnia.[30] Symptoms are more pronounced when the flight is long. Flying east also tends to cause worse symptoms than flying west. Typically, a person requires only one day per time zone to adjust to the new time zone. So, if you have flown from Los Angeles to New York and passed three time zones, you should be fine after three days.
It is possible to reset your circadian rhythm when you travel through time zones. If you are travelling through several time zones, you should adjust your sleep time gradually. Depending on the time zone you need to adjust, you should go to bed half an hour earlier (or later) than usual and also get up half an hour earlier. The next day, go to bed and get up one hour earlier. The day before you travel you should go to bed and get up 90 minutes earlier. On the day of your trip, you should adjust to the new time zone much easier and faster.

Exposing yourself to sunlight should also help tune your inner clock to the new time.[31] If you feel sleepy, avoid caffeine because it will only make your problem worse.
Parasomnias are sleep disorders characterized by an unwanted physical movement, behaviour or action during sleep. The most common parasomnias, also known as abnormal sleep behavior disorders are REM sleep behavior disorder, sleep talking, sleepwalking and nightmares.
The main problem individuals who suffer from REM sleep behavior disorder have is acting out their dreams, which in most cases, leads to self-injuring or injuring another person. What acting out a dream means? For most of us, dreaming is an activity that remains mental, meaning it doesn’t involve any physical movement or talking. Dreams occur in our mind and no matter how vivid and exciting they may be, our body always stays at rest. However, people with RBD physically move their arms and legs or start hitting and punching in bed. While some individuals with RBD often get out of bed and perform different activities that we normally do when we are awake, others talk in their sleep or even shout and scream.

REM sleep behavior disorder is usually noticed when it jeopardizes the safety of the sleeper or his bed partner. Acting out a dream often leads to self-injury. However, in most cases, the bed partner is the one that gets physically hurt, especially if the RBD sufferer kicks and hits in bed.
In order to comprehend RBD, we must be aware that during sleep, we transition between three states – wakefulness, REM sleep, and non REM sleep. Each state and stage of sleep has its own unique characteristics.
REM sleep stage is the most important for understanding this disorder. In REM sleep behavior disorders, the neurological barriers between three main states of sleep break down or misfunction. Due to neurological dysfunction, characteristics of one state invades the other and vice versa. Sleep researchers do not know what affects these neurological barriers and cause them to break down. The neurological barriers between three main stages of sleep are also altered in narcolepsy and parasomnias. Rapid eye movement is characterized by temporary muscle paralysis and associated with dreaming
Since individuals suffering from RBD lack muscle paralysis that normally occurs during REM sleep, they are enabled to act out their dreams. RBD sufferers don’t act out their dreams immediately. Sleep talking or jerking during dreaming can last for years before the symptoms of this disorder fully develop.
Good news for all RBD sufferers is that when the proper diagnosis is set, the condition can be successfully treated. In 90% of the cases, a drug from the group of benzodiazepines, called clonazepam, successfully eliminates REM sleep behavior disorder. The advantage of using this medication is that it doesn’t develop tolerance, even during extended use that lasts for years. If clonazepam doesn’t work, a sleep specialist may recommend antidepressants or melatonin to reduce the violent behavior.
Creating a safe sleep environment is vital to prevent injuries. All sharp or breakable objects from the area near the bed should be removed. The doors and windows in your home should be locked during the night.
Sleep talking is a sleep disorder that is characterized by talking during sleep without being aware of it. Sleep talking can include mumbling, complete nonsense or complicated dialogues or monologues. This sleep disorder is very rare, and in most cases, only a temporary issue. Although anyone can experience sleep talking, it is more common in children and males.
Sleep-talkers are not aware of their speech, so it is not unusual if their voices or type of language sound completely different from wakeful talking. Sometimes, sleep talking can be triggered by conversing with the sleeper. It can also be spontaneous.
When it comes to the content of sleep talking, it may be complete nonsense, or it can relate to past events, and experiences. Sleep experts claim sleep talking is not a product of a conscious or rational mind. Although it’s not physically harmful or dangerous, this sleep disorder can cause embarrassment or annoy a bed partner or a roommate.
Sleep talking is a temporary condition. It may be caused by different external and internal factors, such as stress, sleep deprivation, anxiety, alcohol, fever and so on. External factors typically stimulate the behavior. This disorder can also occur together with nightmares, sleep apnea, and REM sleep behavior disorder. In rarer cases, sleep talking is associated with a mental or medical disease.
Signs of sleep talking can be of different severity and duration and can occur during any stage of sleep. In light sleep, speech is more comprehensible, and in the deeper stages of sleep, the speech is more incomprehensible. The number of sleep talking episodes per night, as well as its duration, determines the severity of the disorder.
Based on severity, sleep talking can be mild, moderate or severe, and based on duration; it can be acute, subacute and chronic.
Apart from talking during sleep, other symptoms may appear, such as sleepwalking, nightmares, sleep apnea, nocturnal seizures, REM sleep behavior disorder, and confusional arousals.
Typically, no treatment is necessary for sleep talking. If you experience this problem for a more extended period, it is best to consult with your doctor and look for an underlying medical explanation. In most cases, sleep talking is triggered by stress or by another undiagnosed sleep disorder.
Practicing good sleep habits such as sleeping eight hours per night and sticking to a regular sleep schedule can reduce the frequency and severity of sleep talking. To reduce sleep talking, also stay away from alcohol, heavy meals and stress.
This sleep behavior disorder is characterized by walking or performing other behaviors while asleep. Somnambulism is much common if a person is sleep deprived. Since sleepwalking occurs during stages of deep sleep, the sleepwalker may have difficulties to be awakened. Individuals affected by this sleep disorder do not remember their sleepwalking incidents.
Symptoms of sleepwalking include sitting up in bed and looking around, walking around the house or outside, and even driving.
It is a common misconception we mustn’t wake up a sleepwalker. A sleepwalker should be awakened. Otherwise, we put his safety in danger.
Other symptoms may include sleep talking, inappropriate behavior such as urinating in closets, screaming, violent attacks on the person trying to awake the sleeper and so on. Inappropriate behavior is more common in children while screaming only occurs when in conjunction with nightmares and sleep terrors.
Causes are mostly unknown. However, sleepwalking can be triggered by sleep deprivation, certain medications with a sedative effect, alcohol, and febrile illnesses. Sleepwalking is mainly experienced by children between the ages of three and seven. Bedwetting and sleep terrors also commonly occur with sleepwalking.
There is no specific treatment for this sleep issue. In many cases, practicing healthy sleep habits eliminates the problem. If the problem persists, your doctor may recommend medical therapy such as sedative-hypnotics or antidepressants. Many adults have successfully treated sleepwalking with hypnosis.
Creating a safe sleep environment is vital to prevent injury during sleepwalking episodes. If your child is sleepwalking, it should not sleep in a bunk bed. All sharp or breakable objects from the area near the bed should be removed. The doors and windows in your home should be locked during the night. Install gates on stairways will also help prevent injury.
Nightmares are dreams with vivid and disturbing content that often causes the sleeper to wake up immediately and recall of the dream. Nightmares are more common in children but can also occur in adults. Sleep terrors are considered extreme nightmares, and they are also typically common in children. However, unlike nightmares that occur during REM sleep, sleep terrors occur during non-REM sleep.

Sleep terrors are accompanied by arousal, agitation, and sweating. The sleeper also has large pupils and increased blood pressure. Usually, the child screams in terror and remains terrified for a few minutes. After they relax, they fall asleep again. The child typically doesn’t remember the dream or has an unclear memory of it.
These sleep disorders are characterized by simple, and repeating movements during sleep or wake. These rhythmic movements often disturb the sleep of the patient and his bed partner. Most common sleep-related movement disorders are restless legs syndrome, periodic limb movement in sleep and teeth grinding or bruxism.
Restless legs syndrome is a sleep disorder characterized by involuntary rhythmic movements of legs while at rest. The desire to move the legs is often followed by unpleasant sensations that are alleviated by movement or pressure.
Since symptoms of are most severe in the evening and during night, they can severely disrupt a patient’s sleep and daily life. Movements can occur periodically or cluster in episodes that can last a few minutes or even a few hours. Restless legs syndrome is not similar to normal muscle spasms that we tend to experience during sleep or while trying to fall asleep.[19]
The causes of this sleep disorder are still unknown. The issue can be caused by other medical conditions such as Parkinson’s disease and narcolepsy. Restless legs syndrome can also be caused by antidepressants.
Symptoms include involuntary leg movements. Sometimes, a partial flexing of the ankle, knee, or hip can occur. The movements can cause a partial or full brief awakening. However, patients are often unaware of the movements.

People have difficulties describing the sensations that make them rhythmically move their legs. Sometimes, the sensations are described as “ants crawling through legs” or “soda running through veins”.
If you are worried you may have RLS, answer the following questions. If most of your answers are “yes”, you should further discuss your symptoms with your health care professional.
If you are sharing a bed with a partner, he or she will notice your problems sooner or later. In fact, restless leg syndrome affects the partner more than the person suffering. Proper diagnosing requires having a polysomnogram test that will record all bodily functions during sleep. Blood work may also be necessary to test your iron status, folic acid, vitamin B12, magnesium levels and so forth.[20]
Restless legs syndrome is a treatable condition. Lifestyle changes are the first step towards alleviating and controlling some of the symptoms.
There is no cure for restless leg syndrome. However, anticonvulsant medications mostly treat restless leg syndrome. Benzodiazepines and narcotics also work well.[21] Doctors and sleep specialists recommend using anti-Parkinson’s type of medicines as the first line of defense because they work the best.[22] Using these drugs significantly reduce or eliminate the symptoms of the disorder.
RLS drugs approved by the FDA are Horizant, Mirapex and Requip. all three drugs are used to treat moderate or severe primary RLS. However, since Requip is used to treat Parkinson disease, it must be given at lower doses.
In addition, there are several medications that are not primarily used to treat RLS, but have been shown to alleviate RLS symptoms. Dopaminergic agonists and agents relieve the symptoms, while benzodiazepines and opiates induce relaxation, relieve unpleasant sensations and ensure less disturbed sleep.
This non-pharmacological treatment includes using a specially designed foot wrap at night in order to relieve the symptoms of RLS. The foot wrap applies continuous pressure to targeted foot muscles and signalizes the brain to relax the muscles of the leg, alleviating symptoms of this sleep disorder.
Studies suggest that RLS symptom relief can be achieved by treating varicose veins in the legs with a non-surgical procedure called sclerotherapy. Sclerotherapy is pain free, and takes about an hour to complete. The patient can immediately walk after the procedure and resume his daily activities. However, this should be done only if your doctor determines that your issue is caused by an underlying vein problem.
In addition to lifestyle changes, a number of self-directed activities can help you manage the symptoms of restless legs disorder. Such activities include walking, stretching, legs massage, hot or cold packs, and similar. Practicing relaxation techniques such as meditation or yoga can also help you alleviate the symptoms.
Periodic limb movement disorder is characterized by involuntary movement of arms and legs. The rhythmic movements typically seem like brief muscle twitches or jerking and occur every 20-40 seconds. The symptoms often cluster into episodes that can last from a few minutes to a couple of hours.
The cause of this sleep disorder is unknown. Doctors and sleep specialists believe an underlying cause exists in the patient’s nervous system. This disorder is not considered very serious. However, since it disturbs sleep, it can lead to daily fatigue or insomnia. In rarer cases, PLMS can be caused by severe medical conditions such as kidney disease or diabetes.
Patients usually experience an irresistible desire to move their arms or legs. Individuals mostly have the urge to move their legs. The urge is often followed by unpleasant sensations in the calves or thighs. These sensations may keep you awake at night or even wake you up from your sleep.
People suffering from PLMS sometimes don’t experience symptoms or aren’t aware of them. The patient’s bed partner is usually the first one who notices these movements.
Physicians recommend treating PLMS only when it’s accompanied by RLS, insomnia, and fatigue. If you think you suffer from periodic leg movement disorder, it is best to consult with your family doctor.
Nocturnal tooth grinding, also known as sleep bruxism is a common condition that affects around 8% of adults. Teeth grinding is more common in children, and it is estimated that approximately 1/3 of parents have a child that experienced symptoms of this condition.
Cause of teeth grinding is mostly unknown. Temporary nocturnal teeth grinding is usually caused by stress. Some studies link bruxism with alcohol consumption, smoking, caffeine, snoring, and fatigue. Some medications such as amphetamines can cause nocturnal teeth grinding. Internal factors do not contribute to bruxism. In most cases, the issue is caused by idiopathic reasons or external factors.
Occasional teeth grinding is not harmful. However, if it occurs regularly, it may lead to permanent dental damage, facial pain, and interrupted sleep. Common symptoms of this condition are worn down teeth, headaches, earaches, sore gums, teeth, and jaw. If the symptoms are severe, the patient can experience interrupted sleep.
If you have bruxism, it is essential to take action before permanent dental damage occurs. You can consult with a sleep expert or your dentist. A sleep specialist will teach you how to reduce stress and relax before bed, while a dentist will make an oral appliance that will protect your teeth from damage.
Since stress and anxiety often cause this condition, it is recommended to minimize it. Symptoms in children usually disappear on their own. For persistent and severe cases, a dentist may suggest wearing an oral appliance that will protect your teeth. Jaw-aligning exercises may also help alleviate the symptoms.
The first toward overcoming a sleep disorder is to identify and track your symptoms carefully. It is also important to track your sleep pattern. To keep track efficiently, downloading a sleep app or keeping a sleep diary should be sufficient.

Your focus should be to pinpoint day and nighttime habits that may be contributing to your sleep problems. Keeping track of your sleep pattern will also be helpful if you decide to visit a doctor. Make sure your sleep diary is as detailed as possible because it can reveal how certain behaviors and activities can prevent you from getting a good night’s rest.
Most sleep disorders such as narcolepsy and sleep apnea require professional help. However, there are also ways you improve your sleeping problems and help yourself.
The first step is to improve your sleep hygiene. Proper sleep hygiene consists of keeping a consistent sleep schedule, healthy stress management[32], healthy eating[33], regular exercising and limiting your intake of drinks and foods that can disrupt your sleep. Limiting alcohol and nicotine is also helpful.
Developing a soothing bedtime routine that helps our mind unwind and prepare to sleep is also important. You should also make sure your bedroom is quiet, dark, and cool[34], and that your bed is comfortable.
If improving your sleep habits didn’t work, it is recommended to visit a sleep specialist or ask your family doctor for help. Schedule an appointment if the following applies to you:
When visiting a doctor, make sure you provide him information from your sleep diary. In order to determine whether or not you have a serious sleep problem that requires medical treatment, a specialist will have to do a polysomnogram test, as well a series of other analyses, such as blood work. After diagnosis, a sleep expert will design a unique treatment program that will alleviate or completely eliminate the symptoms of your sleep disorder.
Resources and references:
[1] http://healthysleep.med.harvard.edu/healthy/matters/consequences
[2] https://www.ncbi.nlm.nih.gov/books/NBK19961/
[3] https://www.cdc.gov/features/dsdrowsydriving/index.html
[4] https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2675894/
[5] https://medlineplus.gov/sleepdisorders.html
[6] https://nccih.nih.gov/health/melatonin
[7] https://www.ncbi.nlm.nih.gov/pubmed/14661186
[8] http://healthysleep.med.harvard.edu/healthy/getting/overcoming/tips
[9] https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3656905/
[10] http://www.sleepeducation.org/treatment-therapy/cognitive-behavioral-therapy
[11] https://www.nhlbi.nih.gov/health-topics/sleep-apnea
[12] http://epworthsleepinessscale.com/
[13] https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3433717/
[14] http://www.stopbang.ca/osa/screening.php
[15] https://www.sleepapnea.com/diagnosis/sleep-apnea-risks
[16] https://www.health.harvard.edu/blog/snored-to-death-the-symptoms-and-dangers-of-untreated-sleep-apnea-2017021311159
[17] https://emedicine.medscape.com/article/1188764-overview
[18]https://www.health.harvard.edu/blog/weight-loss-breathing-devices-still-best-for-treating-obstructive-sleep-apnea-201310026713
[19]https://www.ninds.nih.gov/Disorders/Patient-Caregiver-Education/Fact-Sheets/Restless-Legs-Syndrome-Fact-Sheet
[20] https://emedicine.medscape.com/article/1188327-workup
[21] https://www.drugs.com/condition/restless-legs-syndrome.html
[22] https://emedicine.medscape.com/article/1188327-medication
[23] http://healthysleep.med.harvard.edu/healthy/science/what/sleep-patterns-rem-nrem
[24] https://www.nhs.uk/conditions/narcolepsy/
[25]https://www.ninds.nih.gov/Disorders/Patient-Caregiver-Education/Fact-Sheets/Narcolepsy-Fact-Sheet#3201_3
[26] https://www.xyremhcp.com/xyrem-clinical-trials
[27] https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4050212/
[28] http://www.sleep.theclinics.com/article/S1556-407X(14)00018-6/abstract
[29] https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3020104/
[30] https://www.medicinenet.com/jet_lag/article.htm
[31]https://med.stanford.edu/news/all-news/2016/02/study-finds-possible-new-jet-lag-treatment.html
[32] https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3538178/
[33] http://advances.nutrition.org/content/7/5/938.abstract
[34] https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3427038/
A wannabe journalist who somehow ended up as an art historian. She is a gamer, a coffee addict and a sleep aficionado. When she is not researching about sleep and finding out new ways to fight off the insomnia beast, she's spending time with her friends, gaming or visiting local museums.